Osteoarthritis can affect the knees, hips, wrists, hands or spine. It can also cause pain and stiffness in other joints.
It is important to get a diagnosis, especially if you have been experiencing symptoms for a long time. Your GP may refer you for physiotherapy, podiatry or occupational therapy to help with pain management.
Exercise
Exercise is a vital component of managing OA symptoms. It can strengthen the muscles that support your joints, improve balance and flexibility, and increase overall fitness. It can also help you manage your weight, which can reduce pressure on painful joints. It’s important to talk to a health professional about your exercise program, so that they can ensure it is suitable for you and safe for your joint condition. Osteopath Balwyn North can provide appropriate exercise programs, including strength training, stretching and aerobic exercises on land or water. In some cases, surgery to repair or replace the damaged joint may be required, but this is usually only considered when all other options have been explored.
Although there is no cure for osteoarthritis, regular exercise can keep the joints healthy and flexible, improve muscle strength and energy, limit loss of bone density and maintain a good weight to relieve stress on the joints. If your arthritis is in a weight bearing joint, such as the knee or hip, doing strengthening exercises that target those muscles can be particularly helpful. Exercises that can help include triceps extensions (holding a weight overhead, keeping elbows bent) and side lateral raises. Alternatively, a wall push-up (stand with feet about 12 inches away from a wall and place hands a little wider than shoulders) can be a great option for people who can’t do conventional push-ups.
Massage
Osteoarthritis (OA) develops when the cartilage and other tissues in a joint break down. This usually happens gradually over time, but can be triggered by an injury, or by changing patterns of movement that put stress on the joint (for example, repetitive motions like using a computer keyboard).
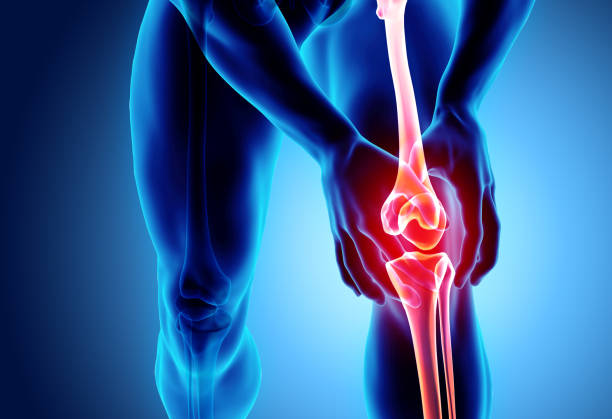
The most common symptoms are pain and stiffness with difficulty moving the affected joint and, sometimes, swelling, tenderness and a crackling sound when you move the joint. Symptoms vary from person to person and different joints are affected. Symptoms can range from mild and come and go to so severe that they stop you doing daily activities, such as getting out of bed, standing on one leg or holding a cup of coffee.
Treatment can include pain relief medicines, physiotherapy, self-management and changes to diet and lifestyle. It’s important to keep up with daily activities, as not enough movement can cause muscle weakness, worsening joint pain and stiffness and increase the risk of further damage to the joint.
In a small number of cases, surgery may be needed to repair, strengthen or replace the damaged joint. This can be done on the knees, hips, elbows, wrists, fingers, toes or spine. This can relieve pain and improve function and quality of life. It is most commonly used in the knees, hips and ankles.
Nutrition
Keeping a healthy weight, regular exercise and eating a balanced diet can help to manage the symptoms of osteoarthritis. A dietary program can include lots of fruit and vegetables, whole grains, low fat dairy and healthy oils (such as olive and canola). Nuts, fish and avocado also contain good amounts of omega-3. Certain foods like garlic and onions contain a component called diallyl disulfide which is known to slow down the deterioration of cartilage.
X-rays and blood tests may be used to look for narrowing of the joints, or other signs of damage to the joints. However, an x-ray doesn’t tell how much pain or stiffness you will have, and some people have little pain from a lot of joint damage.
Early, nonsurgical treatment can maintain joint mobility and improve strength. Most treatment programs combine lifestyle changes, medication and physical therapy. Acetaminophen or other nonsteroidal anti-inflammatory drugs can reduce pain and swelling. Some people need steroid injections directly into the joints to relieve inflammation and pain. Surgery can be helpful if conservative treatments don’t ease pain and improve function. Surgery can involve joining two bones together or replacing the damaged ends of the bone, most often in knees, hips, shoulders, wrists, thumbs and ankles.
Osteoarthritis is one of the most common and most disabling chronic diseases affecting older adults. It can cause pain and stiffness in the joints, especially those used for walking or climbing stairs. The pain tends to come and go, and it’s often worse in the morning or after prolonged rest. The pain may be accompanied by a click, crackle or grinding sound as the joints move, called crepitus.
Sleep
Getting a good night’s sleep can help you cope with the pain and stiffness of osteoarthritis. It’s important to try to go to bed at the same time each night and avoid sleeping in positions that cause joint pressure. It’s also helpful to use pillows to take pressure off painful joints. Using hot or cold packs can help to ease pain and inflammation by increasing blood flow to the affected area.
Regular exercise is one of the best treatments for osteoarthritis. It keeps the joints healthy and flexible, helps you lose weight and can reduce symptoms. However, it’s important not to overdo it as doing too much or doing the wrong sort of exercise can damage your joints.
You may need to see a health professional (such as a GP or a physiotherapist) to get a diagnosis of osteoarthritis and to develop a management plan. This will usually involve lifestyle modifications, medication and/or physical therapy.
NSAIDs (such as ibuprofen and naproxen) can reduce pain, stiffness and swelling. These can be taken as tablets or in a cream, gel or spray. Stronger painkillers such as oxycodone or codeine are sometimes used but are only recommended for short periods because they can have more serious side effects. Occasionally, doctors will inject steroids directly into a joint to relieve pain. This can be for very painful arthritic joints, to relieve sudden severe pain or to treat a specific condition such as gout.









